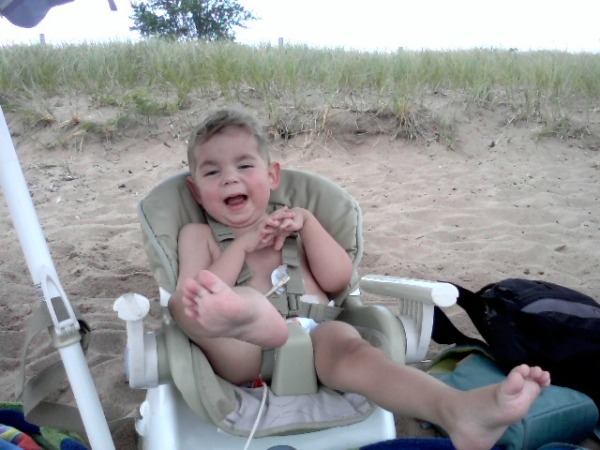
When I haven’t heard Reese chattering over the monitor in the morning, I first feel for his breathing. There is a brief moment of each morning that I wonder what I will find when I go to get him up. To most moms, I know that sounds terrible. That is the reality of living with a disease that the course is unknown.
When Reese first got his diagnosis of “suspected mitochondrial disease complex IV deficiency,” I Dr. Googled all sorts of things. The future looked grim. I prepared for him to die within the first year after his diagnosis. After we resigned to the reality of having a child with very severe disabilities, the question became “how long will he be with us?”
I knew children who were severely disabled and relied on medical technology to stay alive. My mom was a nurse on the pediatric floor and the pediatric intensive care unit for 20 years and my job brought me face to face with what technology could do. I read of families that out of love for their children exhausted the options to keep them alive, many living much of their life in a hospital. I knew that was something I was unwilling to do.
The spring and summer after Reese turned one, we spent 24-7 trying to get calories into him. He lost his ability or willingness to drink from a bottle. We could only feed him his terrible tasting ketogenic diet formula made of cream, oil and baby food with a syringe. Actually, my husband was the only one who could truly “successfully” feed him. We planned where we fed him by how easy it was to clean up the vomit that would happen after a feeding. We were at a crossroads; do we get a feeding tube or not? Was this feeding difficulty due to his GI system shutting down because of his mitochondrial disease (GI systems are HUGE energy users)? Was he so malnourished that he could not keep anything down? Was it something else that was more easily fixable?
To this point, I felt adamant about no feeding tube. I talked with a physician on the ethics board at our hospital when I had the suspicion that we were heading down the feeding tube route. He encouraged me to think about, given this suspected progressive form of mitochondrial disease, what do we want Reese’s death to look like? A cruel question for a mom, but somehow thinking about it seemed right. We had no idea what direction Reese’s path would take.
The decision to not get a feeding tube was met with much criticism. “It’s so easy” moms would say. “Why would you NOT do it?” others would question. I struggled to have a good answer. I feared I was putting less value on Reese’s life because I didn’t want to “tube him.” Somehow I just knew in my heart, I did not want to medicalize Reese’s life and his death any more than we needed to. Reese’s seizures and decreased energy production devastated his brain and cognitive development. I knew that we would have a child reliant on us and his caregivers for the rest of his life. We were (barely) surviving him not having a tube. To start down that medical road of tubes with a relatively “easy” feeding tube seemed a slippery slope that once started was difficult to stop.
Changed minds
In August of 2007, Reese was 1 ½ years old. We were exhausted and he was starving. I called his pediatrician and said “I think we need to think about a feeding tube.” He vomited most of his feedings. He wasn’t gaining weight. We tried all we knew to try. The next thing to try was to bypass his feeding mechanism with a tube. We were unsure of why he was having so much trouble. That evening I talked with our beloved neurologist and he said, “Nena, I think it is time, but if you want to wait a week or a month, I will support your decision.” Had we waited, Reese would not be with us, I am sure of that.
We met with with Reese’s pediatrician; she said Reese could get his feeding tube tomorrow if we consented. The team was contacted and there was a spot on the schedule for him. Reese had lost more weight. I talked with my husband. He felt strongly that we try the tube despite not knowing if it would make Reese’s and our life better. We did. The next week we went on vacation to the MN State Fair.
We realized once Reese’s tube was in his stomach that his stomach did not work well. His formula now goes directly into his small intestine. Our next nutritional step for him is IV nutrition if and when his GI system stops working. We will not do that, just as we will not do a tracheotomy (putting a tube into his neck so a machine can help him breathe). Once his bodily systems are unable to do what they need to support life, we feel it is our job to stop.
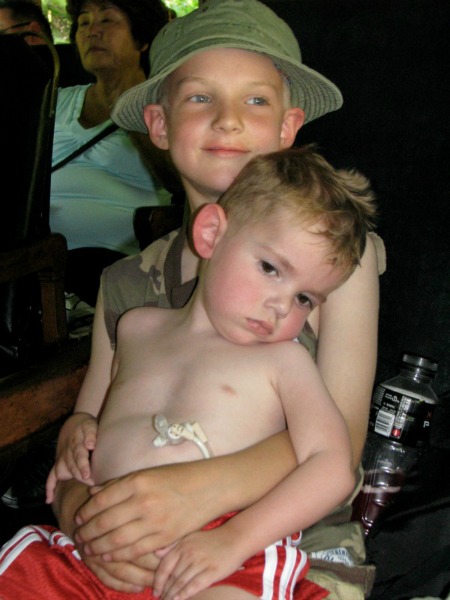 It’s not “easy”
It’s not “easy”
I will never tell a family that getting a feeding tube is “easy” without much qualification. Yes, it makes giving nutrition to a child easy. Eating is the only power struggle that parents can never win, unless their child has a feeding tube. Someone once told me they wished their child had a feeding tube so they could give an unpleasant tasting medicine more easily. I was speechless. Feeding Reese orally was the last “normal” thing that we had to do for him, I grieved that loss. It was far from “easy.”
I know many families go to great lengths to keep their children alive. I do not criticize that, in any way. We all do the best that we can for our children. Our best may look very different than someone else’s. That doesn’t make it wrong, it just makes it different. Our situations can be very similar, but we all come from different backgrounds, beliefs, and understanding. Parents make the best decisions that they can given the information that they have at that very moment.
In the end, I know I will look back and question all of our decisions. That is human nature. I will think of things I could have done better or differently. I do, on the hard days, sometimes wish that we had not gotten Reese’s tube. Many things would be easier if we had made that decision. Many things would be harder. Reese is here because of the decisions we have made and my belief that he will be here as long as he is intended to be.
“You did then what you knew how to do, and when you knew better, you did better.” -Maya Angelou










